
The Top Nationwide Billing Companies You Should Know
Why Choosing the Right USA Medical Billing Services Can Make or Break Your Practice
USA medical billing services are the backbone of financial health for healthcare providers across the country — and choosing the wrong one can cost you tens of thousands in lost revenue every year.
When evaluating nationwide billing companies in 2026, look for these key performance indicators:
Collection Rate: Top-tier firms maintain a 98% or higher collection rate.
Denial Rate: Look for partners that keep denial rates below 2%.
Location: 100% US-based teams ensure better communication and compliance.
Specialty Expertise: Ensure they have experience in 40+ specialties.
The stakes are real. According to the Centers for Medicare & Medicaid Services (CMS), the average claim denial rate in the U.S. sits at 12%, and coding errors alone can drain up to 30% of a practice's revenue. On top of that, 50–65% of denied claims are never reworked — meaning that money is simply left on the table.
Whether you're a solo practitioner or a large multispecialty group, the right billing partner directly impacts how much you collect, how fast you get paid, and how protected your patient data stays.
I'm Olivia Harper, Founder and Denial Management & Reimbursement Specialist of National Billing Institute, with over 30 years of hands-on experience delivering USA medical billing services from our 100% in-office team in Boca Raton, Florida. I've built this guide to help you cut through the noise and find a billing partner that truly protects your revenue.
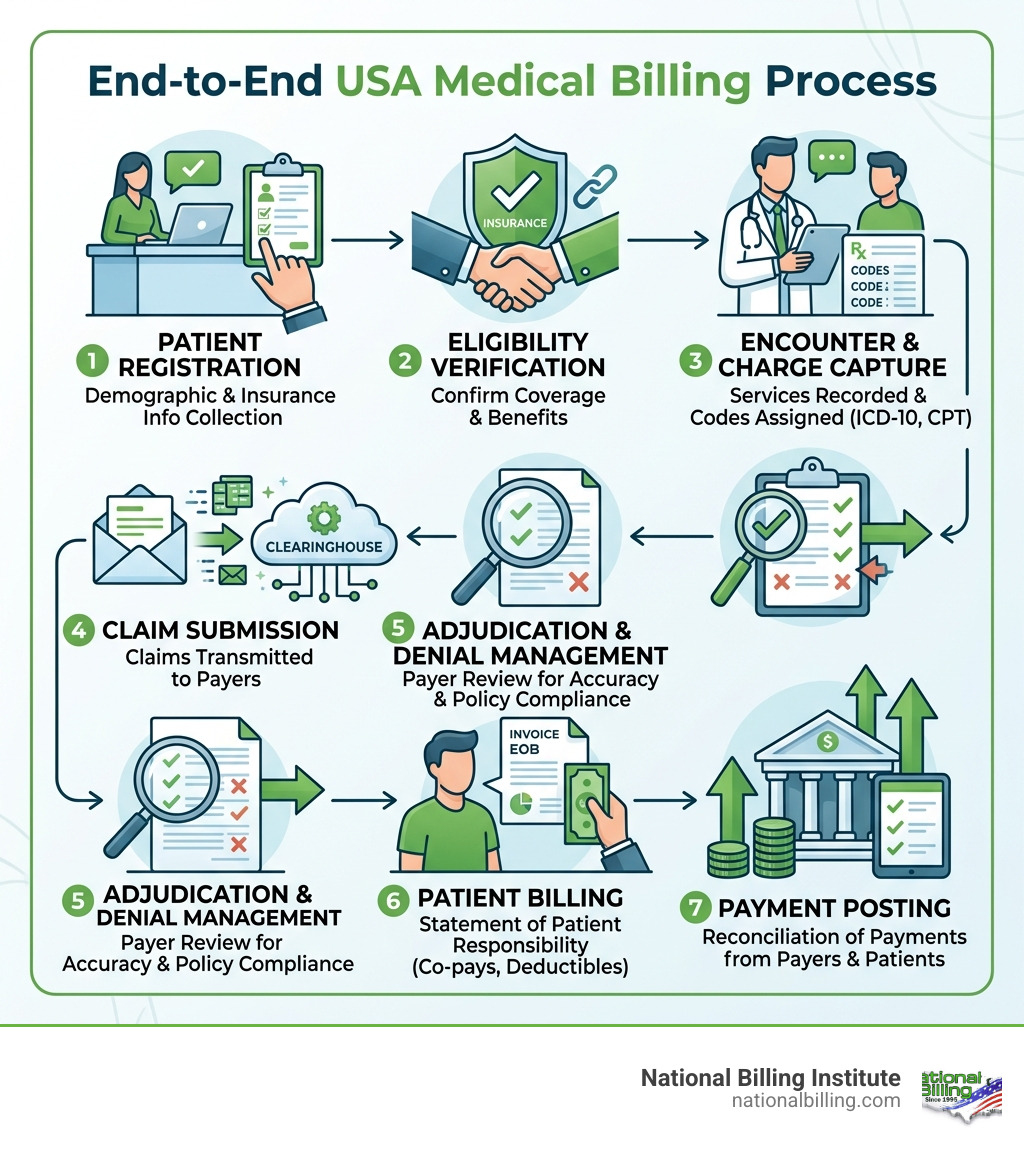
Key Features of Leading USA Medical Billing Services
When we look at the landscape of usa medical billing services in 2026, the "best" companies aren't just those that mail out statements. They are comprehensive partners that manage the entire Revenue Cycle Management (RCM) spectrum. At National Billing, we believe that high-quality Services should act as a protective shield for your practice's hard-earned income.
Leading providers today focus on several non-negotiable pillars:
Certified Coding Expertise: With coding errors potentially causing a 30% revenue loss, top firms employ AAPC or AHIMA-certified coders. These experts navigate the complexities of ICD-10 and CPT codes to ensure every claim is accurate before it ever touches a payer's portal.
Full HIPAA Compliance: In an era of increasing data breaches, 100% HIPAA compliance is the baseline. This includes secure digital encryption for all data transmissions and rigorous internal audits.
Provider Credentialing: You can't get paid if you aren't properly enrolled with payers. Leading services handle the grueling paperwork of CAQH enrollment and payer contracting, ensuring you don't face "out-of-network" denials due to administrative oversight.
MIPS and MACRA Support: Modern billing isn't just about quantity; it's about quality. Top-tier companies help you navigate the Merit-based Incentive Payment System (MIPS), turning regulatory compliance into a financial bonus rather than a penalty.

The Evolution of Revenue Cycle Management in 2026
The world of RCM has changed. In 2026, we aren't just fighting paperwork; we are fighting "algorithmic downcoding." This is where insurance companies use AI to scan your clinical notes and automatically reduce your reimbursement levels.
Currently, the national average for first-pass acceptance rates is roughly 90%. While that sounds high, it means 1 in 10 claims is rejected immediately. Even worse, the average claim denial rate across the U.S. has climbed to 12%. When you consider that 9% of all medical claims are initially denied, the administrative burden on a small practice can be suffocating.
Comparing Software vs. Full-Service USA Medical Billing Services
One of the biggest questions we hear is whether a practice should just buy fancy software or hire a full-service provider.
Software-Based Solutions: Many popular EHR-integrated platforms provide excellent tools for scheduling and patient records. However, they often rely on "ticket systems." If a claim is denied, you might wait weeks for a response from a support rep who doesn't know your practice.
Full-Service RCM Providers: This is what we specialize in at National Billing. We provide a dedicated team that acts as an extension of your office. Instead of a software bot telling you a claim failed, a human expert fixes the error and resubmits it.
Why Choose National comes down to the human element. While software is a tool, a full-service partner provides the strategy needed to navigate the "RCM War of 2026."
Maximizing Revenue with Specialized USA Medical Billing Services
Generic billing is a recipe for underpayment. Different specialties face unique hurdles that require niche expertise:
Cardiology: Requires precise coding for complex procedures and high-level E&M documentation to avoid the 22% spike in denials seen in recent years.
Radiology: With a 95% clean claim rate being the industry goal, radiology billing must account for high volume and specific underpayment recovery.
Mental Health: Practices in this field can see revenue increases of up to 45% simply by improving their Verification of Benefits (VOB) and authorization tracking.
Primary Care: Focuses on closing care gaps and optimizing MIPS scores to ensure maximum Medicare reimbursement.
Pricing Models and the Impact of AI Automation
Understanding how you pay for usa medical billing services is vital for your ROI. In 2026, most companies have moved away from flat monthly fees in favor of performance-based models.
Percentage-Based Fees: Most reputable services charge between 4% and 8% of net collections. If a company offers rates as low as 2% or 2.25%, be sure to ask if they include denial management. Often, "budget" services only submit the claim; they don't fight the denials.
The Pay-for-Paid Model: This is a favorite for many practices because the billing company only makes money when you do. It aligns our goals with yours.
AI and automation are the secret weapons in reducing these costs. AI-driven automation can reduce claim denials by 40% by catching "dumb" errors—like a missing date of birth or an invalid member ID—before the claim is sent. At National Billing, we use these tools to ensure our first-pass rate stays well above the national average.
Overcoming Common Billing Challenges and Denials
The numbers are staggering: 50–65% of denied claims are never reworked. For a practice billing $100,000 a month, a 12% denial rate means $12,000 is at risk. If you don't fight those denials, you are essentially giving the insurance company a "silent tax" on your labor.
Common challenges include:
Coding Errors: These lead to a 30% revenue loss. We solve this by having certified coders perform prospective audits.
Aged Receivables (AR): If your 90-day AR bucket is higher than 15%, your cash flow is in danger. Data-driven analytics can reduce AR days by 35% by identifying which payers are slow-walking your payments.
Credentialing Gaps: Missing a re-credentialing deadline can halt your cash flow for months.
If you aren't sure where your practice stands, you should Schedule Billing Review to identify where your revenue leaks are occurring.
Frequently Asked Questions about USA Medical Billing Services
How do pricing models for medical billing services work in 2026?
Most usa medical billing services use a percentage-of-collections model, typically ranging from 4% to 8%. Some high-volume or specialty-specific firms may offer rates as low as 2.25%. It is important to ensure the rate includes "full-service" RCM, meaning they handle the denial appeals and patient collections, not just the initial claim submission.
What role does AI and automation play in reducing claim denials?
AI is used for "claim scrubbing," which checks for errors against thousands of payer rules in milliseconds. In 2026, advanced services also use NLP (Natural Language Processing) to ensure clinical notes support the level of service billed, which helps combat algorithmic downcoding and can reduce denials by up to 40%.
Why is credentialing and AR recovery vital for practice revenue?
Credentialing ensures you are legally and contractually allowed to receive payments from insurers. Without it, claims are rejected outright. AR recovery is the process of chasing down old, unpaid claims. Effective AR management can increase payment collections by over 30%, turning "lost" money into liquid capital.
Conclusion
Navigating usa medical billing services doesn't have to be a headache. Whether you choose a large national firm or a specialized boutique service, the goal remains the same: maximizing your revenue so you can focus on patient care.
At National Billing Institute, we take pride in being a 100% USA-based team located in Boca Raton, FL. With over 30 years of experience, we’ve seen the industry evolve from paper claims to AI-driven RCM. Our clients typically see a 15-30% revenue increase and enjoy some of the lowest denial rates in the country.
If you’re ready to stop leaving money on the table and want a partner who treats your business like their own, we invite you to learn more about our Company Info or Contact Us today. You can also explore our full range of https://nationalbilling.com/Services to see how we can tailor a solution for your specific specialty. Let's get your practice the revenue it deserves.