
Everything You Need to Know About Telehealth Coding Modifiers
Essential Telehealth Billing Modifiers for Accurate Reimbursement
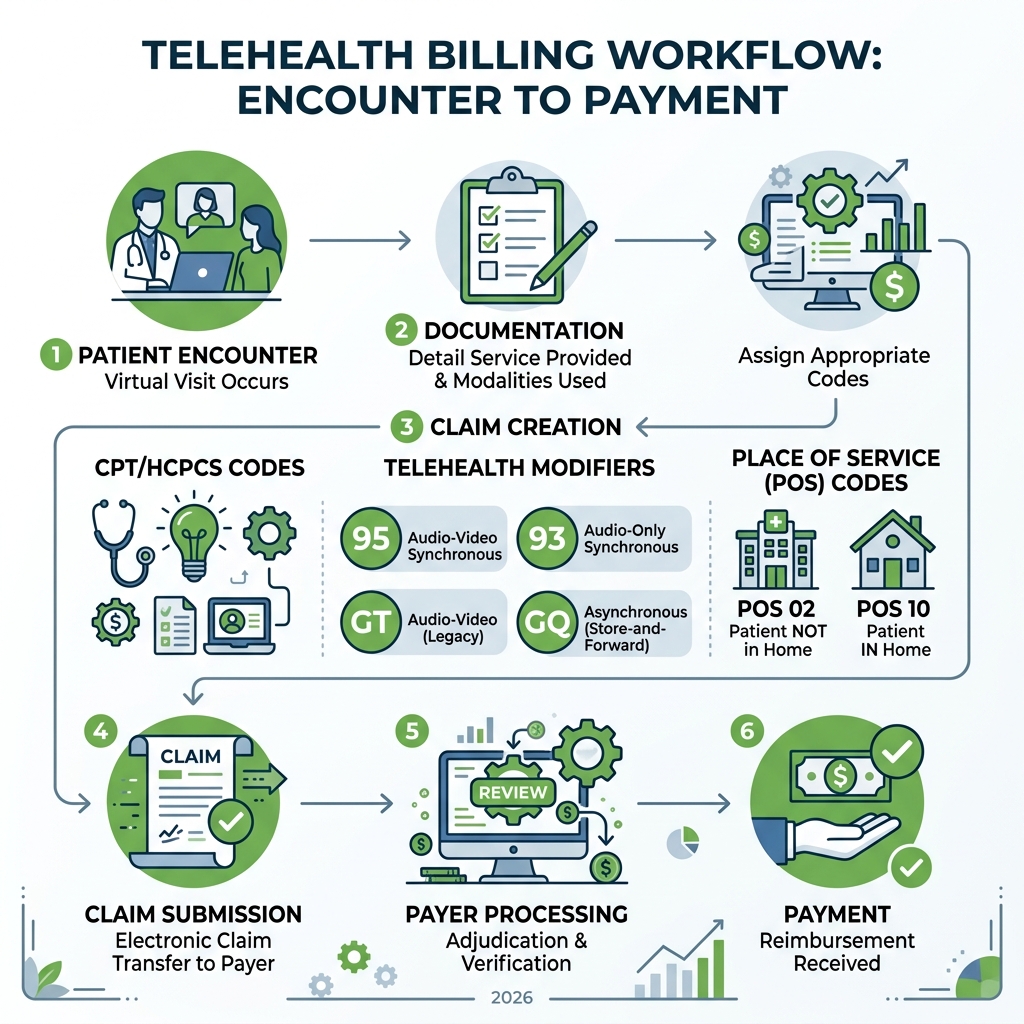
Telehealth billing modifiers are two-character codes appended to CPT or HCPCS codes that tell payers how a telehealth service was delivered — by video, audio-only, or store-and-forward. Getting them right is the difference between a paid claim and a denial.
Quick reference — the most common telehealth billing modifiers:
Modifier Type of Service Primary Use 95 Synchronous audio-video Most commercial payers and Medicare Advantage GT Synchronous audio-video (legacy) CAH Method II institutional claims; some Medicaid 93 Synchronous audio-only Telephone-only visits without video GQ Asynchronous (store-and-forward) Alaska/Hawaii federal demos; some Medicaid FQ Audio-only at home FQHCs, RHCs, behavioral health
These modifiers work alongside Place of Service codes — POS 02 (telehealth outside the patient's home) and POS 10 (telehealth in the patient's home) — to complete an accurate telehealth claim.
Getting this combination wrong is one of the top reasons telehealth claims are denied. And with over 12.6% of Medicare beneficiaries receiving telehealth in just the last quarter of 2023 — and more than 250 codes now eligible for Medicare reimbursement — the stakes have never been higher.
I'm Olivia Harper, Founder and Denial Management & Reimbursement Specialist of National Billing Institute, with over 30 years of experience in revenue cycle management, including deep expertise in telehealth billing modifiers and coding compliance. In this guide, I'll walk you through every modifier you need to know, how payer rules differ, and how to avoid the billing mistakes that quietly drain your revenue.

When we talk about telehealth billing modifiers, we are essentially talking about the "translator" between your clinical work and the insurance company’s checkbook. Without these two little characters, a payer has no way of knowing if you saw the patient in person or via a screen.
The Telehealth service modifiers - FCSO Medicare guide highlights that modifiers are essential for maintaining the integrity of the Medicare Trust Fund while ensuring providers are paid fairly for remote work.
Modifier 95: The Gold Standard for Synchronous Interaction
Modifier 95 is the heavyweight champion of the telehealth world. It indicates a synchronous telemedicine service rendered via a real-time interactive audio and video telecommunications system. If you can see the patient and they can see you, and you are both talking in real-time, 95 is usually your go-to. It is primarily used for codes listed in CPT Appendix P, which covers everything from office visits (99202–99215) to psychotherapy and certain specialty consults.
Modifier GT: The Legacy Legend
Modifier GT used to be the only way to bill telehealth. It stands for "via interactive audio and video telecommunication systems." While Medicare has largely moved away from GT for professional claims—preferring the use of POS codes to trigger telehealth payment—it remains vital for institutional claims, specifically for Critical Access Hospitals (CAH) under Method II. Some state Medicaid programs and older commercial contracts still cling to GT, making it a "legacy" modifier that refuses to retire.
Modifier GQ: The Asynchronous Specialist
Not all telehealth happens in real-time. Asynchronous services, often called "store-and-forward," involve the transmission of recorded medical information (like X-rays, photos, or video clips) to a practitioner who reviews them later. Modifier GQ is the tag for these services. In the Medicare world, this is mostly restricted to federal telemedicine demonstration programs in Alaska and Hawaii, but many state Medicaid plans use it for teledermatology or teleophthalmology.
Comparing Modifier 95 and GT Telehealth Billing Modifiers
The confusion between 95 and GT is real. Think of it this way: Modifier 95 was introduced by the AMA in 2017 to specifically identify synchronous services in the CPT book. GT is a HCPCS modifier.
As we look toward the 2025–2026 telehealth coding updates, the trend is clear:
Professional Services: Use 95 for almost all commercial and Medicare Advantage video visits.
Institutional/CAH Method II: Use GT.
Medicaid: Check your specific state manual; some (like Illinois) still mandate GT for certain encounters to avoid the dreaded EX1i denial code.
Requirements for Audio-Only Telehealth Billing Modifiers (93 and FQ)
Sometimes, the Wi-Fi fails, or the patient simply doesn't have a smartphone. This is where audio-only modifiers come into play.
Modifier 93 was created for synchronous telemedicine services provided via telephone or other audio-only technology. It’s used when the "video" part of the "audio-video" equation is missing.
Modifier FQ is a bit more specific. It indicates a telehealth service was furnished using real-time audio-only technology, typically for behavioral health or mental health services. For Federally Qualified Health Centers (FQHCs) and Rural Health Clinics (RHCs), using FQ is mandatory when the patient is at home and cannot or does not consent to video.
According to Billing and coding Medicare Fee-for-Service claims, you must document that the patient was offered video but chose audio, or that video was technically unavailable, to support the use of these modifiers.
The Critical Role of Place of Service (POS) Codes 02 and 10
While telehealth billing modifiers tell the story of how the service happened, POS codes tell the story of where it happened. Since 2022, we’ve had two primary choices:
POS Code Description Reimbursement Impact 02 Telehealth Provided Other than in Patient’s Home Often pays at the "Facility" rate (lower) 10 Telehealth Provided in Patient’s Home Pays at the "Non-Facility" rate (higher/same as office)
The Telehealth Billing and Coding: CPT Codes and Place-of-Service Rules | National Telehealth Authority explains that POS 10 was a game-changer. It recognized that providing care to a patient in their private residence involves different overhead and complexity than seeing them in a clinical setting.
Interaction Between POS Codes and Telehealth Modifiers
This is where many practices trip up. You cannot just use a modifier and hope for the best. You must pair the POS code with the correct modifier based on the payer's rules. For example, Optum Behavioral Health recently mandated that all telehealth claims must include either POS 02 or POS 10 effective late 2023. If you bill a telehealth visit with POS 11 (Office), it will likely be denied because the location and the service modality don't match.
At National Billing, we see "Modifier Fatigue" where billers get overwhelmed by these combinations. Our Services include AI-automated scrubbing that ensures POS 10 is never paired with an incompatible modifier, saving our clients from thousands of dollars in "EX1i" (Missing Modifier) errors.
Payer-Specific Guidelines for Medicare, Medicaid, and Commercial Plans
If only every payer followed the same rules! Unfortunately, the telehealth landscape is a patchwork of federal, state, and private policies.
Medicare Fee-for-Service (FFS)
Medicare is actually one of the "simpler" ones now. For most professional telehealth services, Medicare wants you to use the appropriate POS code (02 or 10). They have largely waived the requirement for modifier 95 on professional claims through 2024, though it doesn't hurt to include it. However, if you are billing for audio-only mental health, you must use modifier FQ or 93.
The MLN901705 - Telehealth & Remote Monitoring - CMS PDF is the "bible" for these rules. It reminds us that for 2025 and 2026, many of the COVID-era flexibilities—like allowing the patient to be at home—have been extended, but the billing requirements are becoming more formalized.
State Medicaid Variations
Medicaid is where things get wild. Some states require modifier 95, some require GT, and some require both a modifier and a specific HCPCS code. For instance, Illinois Medicaid is famous for denying claims that don't have GT or 93 attached to POS 02/10. Always check your state-specific provider manual.
Commercial Payer Variations for Telehealth Modifiers
Commercial giants like Aetna, UnitedHealthcare (UHC), and Blue Cross Blue Shield (BCBS) usually follow the AMA guidelines, meaning they want modifier 95 for synchronous video. However, they often have different rules about "payment parity"—whether they pay the same for telehealth as they do for in-person visits.
Because these rules change quarterly, we recommend providers schedule a billing review to ensure their software is updated with the latest payer-specific edits.
Common Telehealth Billing Mistakes and Documentation Requirements
We’ve processed millions of claims at National Billing Institute, and we’ve seen it all. Here are the "Hall of Fame" mistakes for telehealth billing modifiers:
Using POS 11 for Telehealth: This is the #1 mistake. Even if you are sitting in your office, if the patient is at home, the Place of Service is 10.
Missing Audio-Only Modifiers: Billing a 99441 (telephone E/M) without modifier 93 often leads to a "missing information" denial.
The "One-Size-Fits-All" Approach: Assuming that because Aetna accepted modifier 95, Cigna will too. (Hint: They might, but don't bet your cash flow on it).
Double-Billing RPM and Telehealth: Remote Patient Monitoring (RPM) is not telehealth. Don't append telehealth modifiers to RPM codes like 99454.
Industry analysis shows that these "small" errors lead to massive audits.
Documentation Best Practices to Support Telehealth Claims
Your claim is only as good as your note. If an auditor comes knocking, they aren't looking at your modifiers; they are looking at your documentation. To support telehealth billing modifiers, your notes must include:
A Statement of Technology: "Service provided via HIPAA-compliant synchronous audio-video platform."
Location of Both Parties: "Provider is in Boca Raton, FL; Patient is at their private residence in Miami, FL."
Patient Consent: Documentation that the patient agreed to a virtual visit.
Clinical Necessity: Why was telehealth appropriate for this specific encounter?
Total Time: Especially if billing based on time (essential for many E/M and behavioral health codes).
The Telehealth Coding and Billing: Basics - AAFP suggests using a standard template for all telehealth visits to ensure these five elements are never missed.
The Future of Telehealth Coding: 2025-2026 Outlook
As we move into 2025 and 2026, the "temporary" nature of telehealth is vanishing. It’s becoming permanent.
The Advancing Mental Health Act and other legislative moves have made mental health telehealth permanently unrestricted by geography. This means the patient can be anywhere in the U.S., and as long as you are licensed in their state, you can bill Medicare.
However, we expect to see a "narrowing" of audio-only flexibilities. While 2024 allowed audio-only for almost anything due to the tail-end of PHE (Public Health Emergency) rules, 2026 will likely see Medicare restrict audio-only to very specific behavioral health and home-based scenarios.
Starting in CY 2026, Medicare will only add services to the telehealth list on a permanent basis. No more "provisional" codes. This is great news for stability, but it means your billing team needs to be sharper than ever. This is why choose National Billing—we stay ahead of these regulatory curves so you don't have to.
Frequently Asked Questions about Telehealth Modifiers
What is the difference between modifier 95 and modifier 93?
Modifier 95 is for video + audio (synchronous). Modifier 93 is for audio-only (telephone). If the camera is on, use 95. If the camera is off, use 93.
When should I use POS 10 instead of POS 02?
Use POS 10 if the patient is in their "private residence" (this includes a hotel or even their car if they are parked for privacy). Use POS 02 if the patient is anywhere else—like a satellite clinic, a nursing home, or a hospital.
Does Medicare still require the GT modifier for professional claims?
Generally, no. For standard Part B professional claims, Medicare uses the POS code to identify the service as telehealth. However, if you are a Critical Access Hospital billing under Method II, the GT modifier is still your best friend.
Conclusion
Navigating telehealth billing modifiers doesn't have to feel like learning a foreign language. By understanding the core differences between 95, GT, and 93, and pairing them correctly with POS 10 and 02, you can protect your practice from denials and audits.
At National Billing Institute, we specialize in taking the "coding headache" off your plate. Our 100% USA-based team in Boca Raton uses AI-automated processing to catch modifier errors before they ever leave our system. The result? The lowest denial rates in the industry and a 15-30% average increase in revenue for our clients.
Ready to optimize your telehealth revenue? Contact Us for a Telehealth Billing Consultation or visit our Company-Info page to learn how we can help your practice thrive in the digital era. Let’s make sure you get paid for every minute of care you provide, whether it's across an exam table or across a screen.