RCM Medical Coding: The Biller's Best Kept Secret
What RCM Medical Coding Really Means for Your Practice's Bottom Line
RCM medical coding is the process of translating clinical documentation — diagnoses, procedures, and services — into standardized codes that insurers use to process and pay claims.
Here's a quick breakdown of what that means in practice:
Term What It Means RCM Revenue Cycle Management — the full financial journey from patient registration to final payment Medical Coding Converting clinical notes into ICD-10, CPT, and HCPCS codes Why It Matters Coding errors are the #1 driver of claim denials Accuracy Standard Certified coders are held to a 97% accuracy rate The Stakes Healthcare institutions spent $19.7 billion in 2022 just appealing denied claims
In short: if your coding is off, your reimbursements suffer. It's that simple.
Every time a patient walks through your door, a financial clock starts ticking. That visit has to move through registration, insurance verification, documentation, coding, claim submission, and finally — payment. Medical coding sits right in the middle of that chain. Get it right, and claims flow. Get it wrong, and you're fighting denials, writing appeal letters, and leaking revenue.
The U.S. RCM market was valued at $141.61 billion in 2024 and is projected to nearly double to $272.78 billion by 2030. That growth reflects just how critical — and complex — revenue cycle management has become for healthcare providers of every size.
I'm Olivia Harper, Founder of National Billing Institute and a denial management and reimbursement specialist with over 30 years of hands-on experience in RCM medical coding and billing. In that time, I've seen how the right coding practices can transform a practice's financial health — and how coding mistakes can quietly drain revenue for months before anyone notices.
The Critical Role of RCM Medical Coding in Healthcare
Think of rcm medical coding as the universal translator of the healthcare world. When a physician spends 20 minutes treating a patient for hypertension and performing an EKG, those actions exist as ink on a page or digital notes in an EHR. Payers like Medicare or BlueCross don't cut checks based on "notes"; they pay based on specific, alphanumeric codes.

In the broader context of Revenue Cycle Management (RCM), coding is the bridge between clinical care and financial reimbursement. Without this bridge, the data flow stops, and so does the cash flow. At National Billing, we view coding not just as a clerical task, but as a strategic pillar of financial stability. By ensuring Services are documented and coded with 100% integrity, we protect the provider's hard-earned revenue.
Defining the Impact of RCM Medical Coding
The impact of coding ripples through every department. It starts with clinical documentation—if the doctor doesn't write it down, the coder can't code it. This leads to "charge capture," where every billable item is accounted for.
When coding is handled poorly, "revenue leakage" occurs. This is the slow bleed of money that should have been yours but was lost because a code was too vague or a modifier was missing. To prevent this, the industry gold standard is a 97% accuracy rate. Falling even a few percentage points below this can result in thousands of dollars in lost revenue every month.
Why Accuracy is the Number One Driver of Denials
It is a startling fact: coding is the number one reason claims are denied. Currently, about 15% of private payer claims face an initial denial. While that might sound like a small number, the administrative cost to fight those denials is astronomical. In 2022 alone, healthcare institutions spent $19.7 billion just on the appeals process.
The goal is always "first-pass acceptance"—getting the claim paid the very first time it hits the payer's system. According to CMS coding guidelines, accurate coding must prove "medical necessity." If the code for the diagnosis doesn't justify the code for the procedure, the payer will reject it instantly.
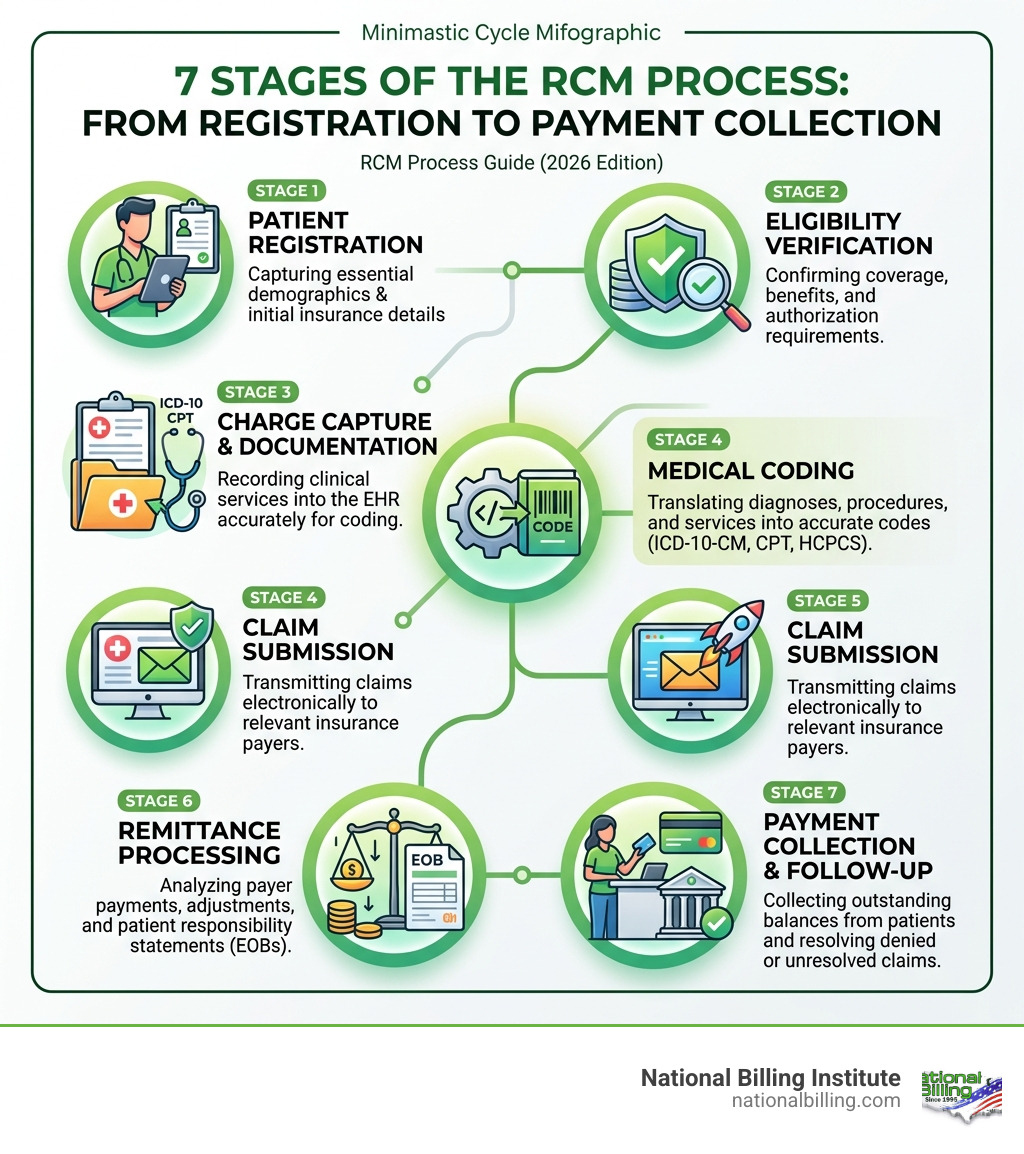
Key Stages and Systems in the Revenue Cycle
Managing the revenue cycle is like running a relay race.
Front-End: Patient registration and insurance verification.
Mid-Cycle: Clinical documentation and rcm medical coding.
Back-End: Claim submission, payment posting, and denial management.
To keep this race on track, we use three primary standardized coding systems.
Standardized Systems for RCM Medical Coding
System Full Name Primary Use ICD-10-CM International Classification of Diseases, 10th Revision Used to describe diagnoses (why the patient is here). CPT Current Procedural Terminology Used to describe procedures and services (what was done). HCPCS Level II Healthcare Common Procedure Coding System Used for supplies, equipment, and drugs not in CPT.
These systems operate under HIPAA 5010 standards to ensure electronic transactions are uniform across the country. Understanding "Modifier usage"—two-digit additions to codes—is also vital. They tell the payer, "Yes, we did this procedure, but there was a special circumstance." When you Why Choose National, you get a team that knows these nuances inside and out.
How RCM Medical Coding Prevents Front-End Errors
While coding happens in the middle of the cycle, it is heavily dependent on the front end. Believe it or not, 23.9% of claim denials are caused by errors during the front-end process, such as mistyped patient names or incorrect insurance IDs.
By integrating coding logic into the registration phase—verifying that the insurance covers the specific codes likely to be billed—practices can stop denials before they even happen.
Overcoming Common Coding Challenges and Denials
Even the best practices face challenges. The most common "red flags" that trigger audits or denials include:
Up-coding: Billing for a more expensive service than what was actually performed (a major compliance risk).
Unbundling: Billing multiple codes for parts of a procedure that should be covered under a single "comprehensive" code.
Under-coding: Leaving money on the table by failing to bill for the full complexity of the work performed.
To navigate these, we rely on CCI (Correct Coding Initiative) edits and LMRP (Local Medical Review Policy) standards. These are the "rulebooks" payers use to decide if codes can be billed together. At National Billing, our Company Info reflects our commitment to staying ahead of these shifting rules.
Strategies to Reduce RCM Medical Coding Errors
We don't leave accuracy to chance. To maintain our "lowest denial rate" reputation, we implement several layers of protection:
Regular Audits: We internalize the "audit" process, checking our own work before the payer does.
Staff Education: Continuous training on new 2025-2026 guidelines.
Clinical Documentation Improvement (CDI): Working with providers to ensure their notes are detailed enough to support high-level codes.
Claim Scrubbing: Using software to "pre-screen" claims for errors before they are sent.
The Role of AI and Automation in Modern Coding
The future of rcm medical coding is here, and it's powered by AI. We are seeing a massive shift toward "Agentic AI" and autonomous coding. These tools can read a physician's progress note and suggest the most accurate codes instantly.
Organizations that implement comprehensive RCM automation see up to a 40% reduction in claim processing time and a 25% improvement in first-pass acceptance. As we move into 2025, CMS updates are increasingly favoring these tech-driven efficiencies, allowing our Boca Raton-based team to focus on complex "human-in-the-loop" decisions while the AI handles the routine heavy lifting.
Professional Standards and Career Pathways
You wouldn't want an uncertified surgeon, and you shouldn't want an uncertified coder. The two main bodies governing this profession are the AAPC (American Academy of Professional Coders) and AHIMA (American Health Information Management Association).
Common credentials include:
CPC (Certified Professional Coder): The gold standard for physician office coding.
CCS (Certified Coding Specialist): Often focused on hospital/inpatient environments.
A great coder needs more than just a certificate; they need a deep understanding of medical terminology, human anatomy, and pharmacology. They have to understand what the doctor did to know how to code it.
Frequently Asked Questions about RCM Coding
What are the most common medical coding errors?
The "big four" are missing or misused modifiers, using an incorrect Point of Service (POS) code, unbundling services that should be grouped, and failing to link the diagnosis to the procedure to prove medical necessity.
How does outsourcing medical coding benefit providers?
Outsourcing to a 100% USA-based team like ours reduces your in-house overhead (no more paying for expensive coding software or benefits for extra staff). It gives you instant access to certified experts and typically results in a 25% improvement in first-pass payment rates.
What KPIs should practices track for coding success?
You should keep a close eye on your Days in Accounts Receivable (AR) (the lower, the better), your Denial Rate (aim for under 5%), and your Clean Claim Rate. These numbers tell the true story of your practice's financial health.
Conclusion
At the end of the day, rcm medical coding is about more than just numbers and letters. It’s about ensuring that your practice remains financially viable so you can continue to provide top-tier care to your patients.
With over 30 years of experience, the team at National Billing Institute in Boca Raton, FL, specializes in turning the "secret" of great coding into a reality for our clients. Our 100% USA-based team is dedicated to HIPAA compliance and helping providers achieve a 15-30% revenue increase by simply doing things the right way.
Stop letting denials drain your hard-earned income. Optimize Your Revenue with National Billing Institute today and see what happens when expert coding meets cutting-edge AI.