
The Secret Sauce to HIPAA Compliant Healthcare Billing
Why Medical Billing HIPAA Compliance Can Make or Break Your Practice
Medical billing HIPAA compliance means protecting patient health information at every step of the billing process — from registration to final payment — while meeting federal standards for privacy, security, and breach response.
Here's what HIPAA-compliant medical billing requires:
Requirement What It Means Privacy Rule Limit who can see and use patient data Security Rule Protect electronic records with safeguards Business Associate Agreements Written contracts with all vendors handling PHI Minimum Necessary Standard Only access the data you actually need Breach Notification Report incidents within 60 days (possibly 24 hours by 2026) Staff Training Annual training for everyone who touches patient data
Most practices assume HIPAA violations come from hackers. They don't. Over 176 million patients have had their health information exposed — and most breaches came from employee mistakes, not outside attacks.
Consider what happened to a Florida medical billing company in 2023. They sent patient files by regular email instead of encrypted channels — just to save time. Six months later, after penalties, lawsuits, and lost clients, they shut down permanently. 2.7 million patient records exposed. Gone.
The stakes are real. Civil penalties run from $100 to $50,000 per violation, up to $1.5 million per year. Criminal violations can mean prison time.
I'm Olivia Harper, Founder of National Billing Institute, and with over 30 years of hands-on experience in medical billing HIPAA compliance and revenue cycle management, I've seen how the right compliance framework protects both patients and practice revenue. In this guide, I'll walk you through exactly how to implement HIPAA billing standards — step by step.
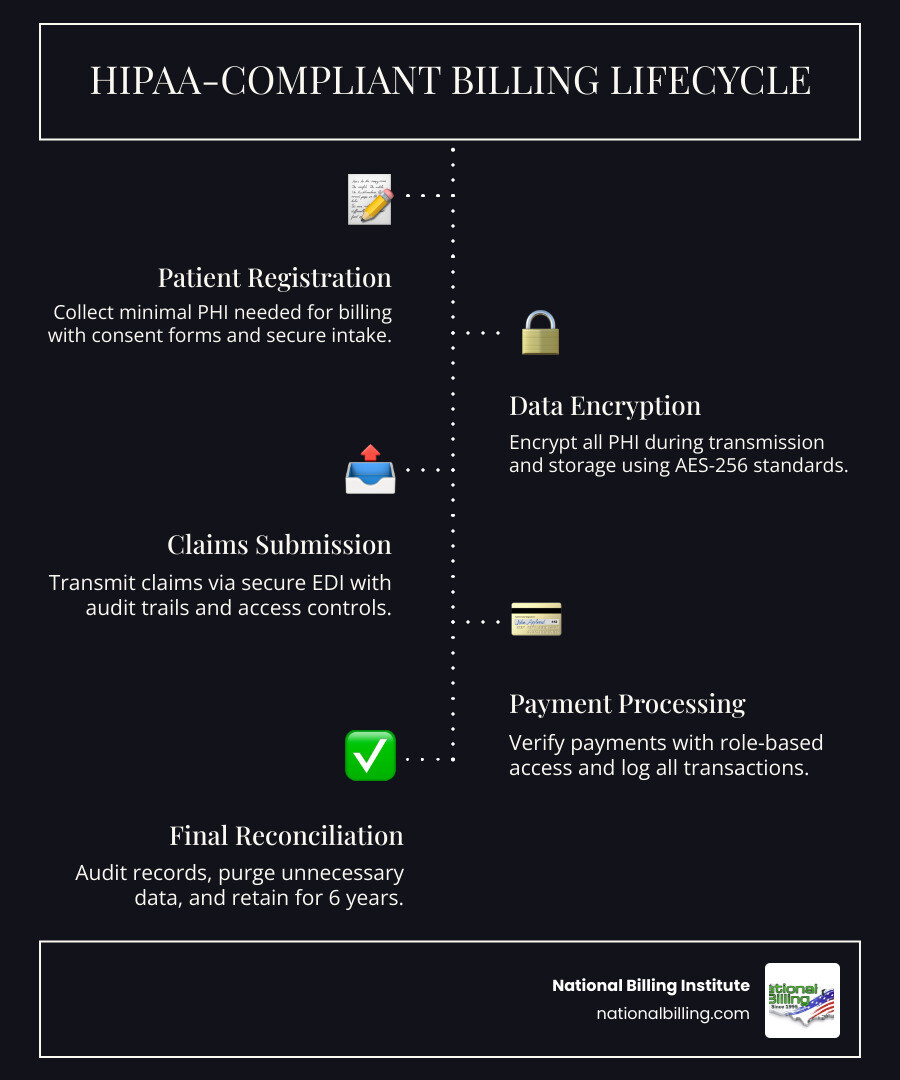
Understanding the Pillars of Medical Billing HIPAA Compliance
To master medical billing HIPAA compliance, we first have to look at the two heavy hitters: the Privacy Rule and the Security Rule. Think of the Privacy Rule as the "who" and "what" (who can see the data and what data is protected), while the Security Rule is the "how" (how we lock the digital doors).

The Privacy Rule, which took effect in 2003, sets the national standards for when Protected Health Information (PHI) can be used or shared. In the billing world, this means we have permission to use PHI for "payment" purposes without a specific patient sign-off every single time, but we are still bound by strict limits.
The Security Rule, arriving in 2005, focuses specifically on electronic PHI (ePHI). It demands that any entity handling digital billing data—whether a doctor's office in Boca Raton or a clearinghouse—implements specific administrative, physical, and technical safeguards.
For a deeper dive into these regulations, you can explore How HIPAA Compliance Affects Medical Billing.
Privacy Rule vs. Security Rule: The Billing Perspective
Feature HIPAA Privacy Rule HIPAA Security Rule Focus All PHI (Paper, Oral, Electronic) Electronic PHI (ePHI) only Goal Protect patient privacy and rights Ensure data confidentiality, integrity, and availability Billing Application Controls who the biller talks to about a claim Dictates the encryption used to send that claim Patient Rights Right to access and amend records N/A (Technical focus)
Defining PHI and ePHI in the Billing Process
In our line of work, we handle more than just names. PHI includes any information that can link a specific individual to their health status or payment for care. There are 18 specific identifiers that turn "data" into "PHI."
For medical billers, this includes:
Patient Names and Addresses: The basics for sending statements.
Social Security Numbers: Often used for identity verification.
ICD-10 and CPT Codes: These are "fingerprints" of a patient's medical history.
Payment History: Even the fact that someone owes money to a specific specialist is protected.
Dates: Birth dates, admission dates, and discharge dates.
Data only becomes "safe" for general use once it is fully de-identified, meaning all 18 identifiers are scrubbed so the person can no longer be identified.
The Role of Business Associate Agreements (BAAs)
If you aren't doing your billing entirely in-house, you are likely working with a "Business Associate." This could be a software vendor, a shredding company, or a professional service like ours.
A Business Associate Agreement (BAA) is a legally binding contract that ensures these third parties follow the same strict HIPAA rules you do. Without a BAA in place, sharing a single patient record with a vendor is a violation. At National Billing, we take this a step further by ensuring all our downstream subcontractors—like the cloud servers we use—are also bound by these same protections. You can learn more info about secure billing services to see how we handle these contractual obligations.
Essential Safeguards for Protecting Patient Data
Compliance isn't a "set it and forget it" task. It requires a three-layered shield of safeguards: Administrative, Physical, and Technical.
The Office for Civil Rights (OCR) doesn't just look for a lack of breaches; they look for a lack of safeguards. A practice can be fined millions just for failing to conduct a "risk analysis," even if no data was actually stolen. For more on these requirements, check out HIPAA Compliance for Billing Companies: Requirements and Best Practices.
Technical Controls for ePHI Security
This is where the rubber meets the road in the digital age. If we are sending claims across the internet, we must ensure they are unreadable to anyone but the intended recipient.
256-bit AES Encryption: This is the gold standard for data at rest and in transit.
Multi-factor Authentication (MFA): Requiring a password plus a code sent to a phone prevents 99% of unauthorized access.
Audit Logs: We track every single person who views a record. If a biller looks at a celebrity's file out of curiosity, the audit log will catch them.
Automatic Logoffs: If a biller steps away for coffee, the system should lock the screen after a few minutes of inactivity.
Unique User IDs: No shared "Admin" passwords. Every person has their own login.
Physical and Administrative Protocols
You can have the best encryption in the world, but it won't matter if a visitor can see a computer screen in the billing office.
Workstation Security: We use privacy screens on monitors so they can't be read from an angle.
Facility Access: Only authorized personnel should be in the billing area.
Sanction Policies: Employees must know that violating HIPAA has consequences, up to and including termination.
Incident Response: If a laptop is stolen, do you have a plan? You must be able to document that the laptop was encrypted to avoid a massive fine.
How to Implement HIPAA Standards in Your Billing Workflow
Implementing medical billing HIPAA compliance into your daily routine doesn't have to be a headache. It starts with the "Minimum Necessary Standard." This means that if a biller only needs to see the CPT code to file a claim, they shouldn't be reading the doctor's full clinical notes about the patient's personal life.
We recommend using a checklist to ensure nothing falls through the cracks:
Verify Identity: Use two identifiers before discussing a bill over the phone.
Secure Transmission: Never send PHI via standard email.
Authorization: Ensure you have a signed Notice of Privacy Practices on file.
Audit: Review your access logs monthly to spot weird patterns.
To see how we integrate these into our workflows, you can read about why choose National for compliant billing.
In-House vs. Outsourced Medical Billing HIPAA Compliance
There is a common myth that outsourcing your billing removes your liability. It doesn't. While the billing company is directly liable for their own mistakes, the healthcare provider is still responsible for vetting that company.
In-House: Your team is under your direct authority. No BAA is needed for your own employees, but you are 100% responsible for their training and any mistakes they make.
Outsourced: You must have a BAA. The billing company (like us!) brings specialized security expertise, but you must still monitor their compliance.
Our team is 100% USA-based in Boca Raton, FL, which means we operate under the same federal and state jurisdictions you do, providing a much higher level of oversight than offshore teams. You can find more about our background in our Company Info.
Documentation and Record Retention Requirements
HIPAA requires that you keep all compliance-related documentation—policies, training records, and BAAs—for at least six years. However, don't delete everything on year seven!
OSHA: Requires keeping some records for 30 years.
CMS: Often mandates five to six years depending on the facility type.
State Laws: Florida may have specific statutes of limitations that require longer retention.
Always check your local requirements before hitting "delete" on old billing data.
Navigating Penalties and 2026 Compliance Trends
The "Enforcement Rule" is the part of HIPAA that gives the law its teeth. The OCR has become increasingly aggressive in collecting settlements.
Recent history is full of cautionary tales:
University of Texas MD Anderson Cancer Center: Faced a $4.3 million penalty for failing to encrypt devices that were later lost.
UCLA Health System: Paid $865,000 because employees were "snooping" on celebrity records.
Advocate Health Care: Paid $5.5 million after unencrypted laptops were stolen from cars.
If you are worried about where your practice stands, you can Contact Us for a compliance audit to identify vulnerabilities before the OCR does.
The Future of Compliance in 2026 and Beyond
As we move through 2026, the landscape is shifting toward automation and speed.
AI-Automated Claims: We use AI to speed up billing, but this requires new types of risk assessments to ensure the AI isn't "learning" from PHI in a way that violates privacy.
24-Hour Breach Notification: While the current window is 60 days, there is a strong push to shrink this to 24 hours for major breaches.
Telemedicine: With the explosion of remote care, billing for these services requires secure, end-to-end encrypted platforms.
Blockchain: Some experts predict blockchain will become the standard for "immutable" audit logs that can never be altered or erased.
Frequently Asked Questions about Medical Billing HIPAA Compliance
What is the difference between in-house and outsourced medical billing HIPAA compliance?
In-house teams are part of the "Covered Entity," meaning they fall under your direct workforce policies. Outsourced companies are "Business Associates." The main difference is that with an outsourced partner, you must have a BAA in place, and the vendor is legally responsible for their own technical safeguards.
How long must documentation be retained for medical billing HIPAA compliance?
Federal HIPAA rules require six years of retention for documentation of policies and actions. However, we often recommend longer periods—up to 10 years for certain financial records or 30 years for records governed by OSHA—to ensure you are covered for all legal and tax audits.
What are the most common HIPAA violations in medical billing?
The "Big Three" are:
Unencrypted Communication: Sending a bill via a standard Gmail or Outlook account.
Snooping: Staff looking at records of friends, family, or neighbors without a billing reason.
Improper Disposal: Putting paper bills in the regular trash instead of a cross-cut shredder.
Conclusion
At the National Billing Institute, we believe that medical billing HIPAA compliance is the foundation of a healthy revenue cycle. Based in Boca Raton, FL, our 100% USA-based team combines 30+ years of experience with cutting-edge AI-automated claims processing to deliver the lowest denial rates in the industry.
We don't just process claims; we protect your reputation and your bottom line. By implementing the safeguards we've discussed today, you can increase your revenue by 15-30% while sleeping soundly knowing your patient data is secure.
Start your HIPAA-compliant billing journey today and let us show you the "secret sauce" to a worry-free practice.