
The Best Healthcare Claims Processing Systems Reviewed
Why Claims Processing Software Healthcare Decisions Can Make or Break Your Revenue Cycle
Claims processing software healthcare teams rely on has become one of the most critical decisions a practice can make - it directly affects how fast you get paid, how often claims are denied, and how well your staff can keep up.
In 2026, the most effective systems prioritize AI-native workflows, high clean claim rates, and enterprise-level scalability. Whether you are a small practice or a large health system, the goal remains the same: reducing administrative burden while maximizing financial stability.
Claim denials, slow payments, and administrative overload are not just frustrating - they cost practices real money every month. The right software can close that gap fast.
But with dozens of platforms on the market, choosing the wrong one is an expensive mistake.
This guide breaks down the best healthcare claims processing systems available in 2026, what to look for, and how to match the right tool to your practice's needs.
I'm Olivia Harper, Founder of National Billing Institute and a denial management specialist with over 30 years of hands-on experience navigating claims processing software healthcare practices depend on for financial stability. In that time, I've seen which systems reduce denials and which ones create more headaches than they solve.
What is Claims Processing Software in Healthcare?
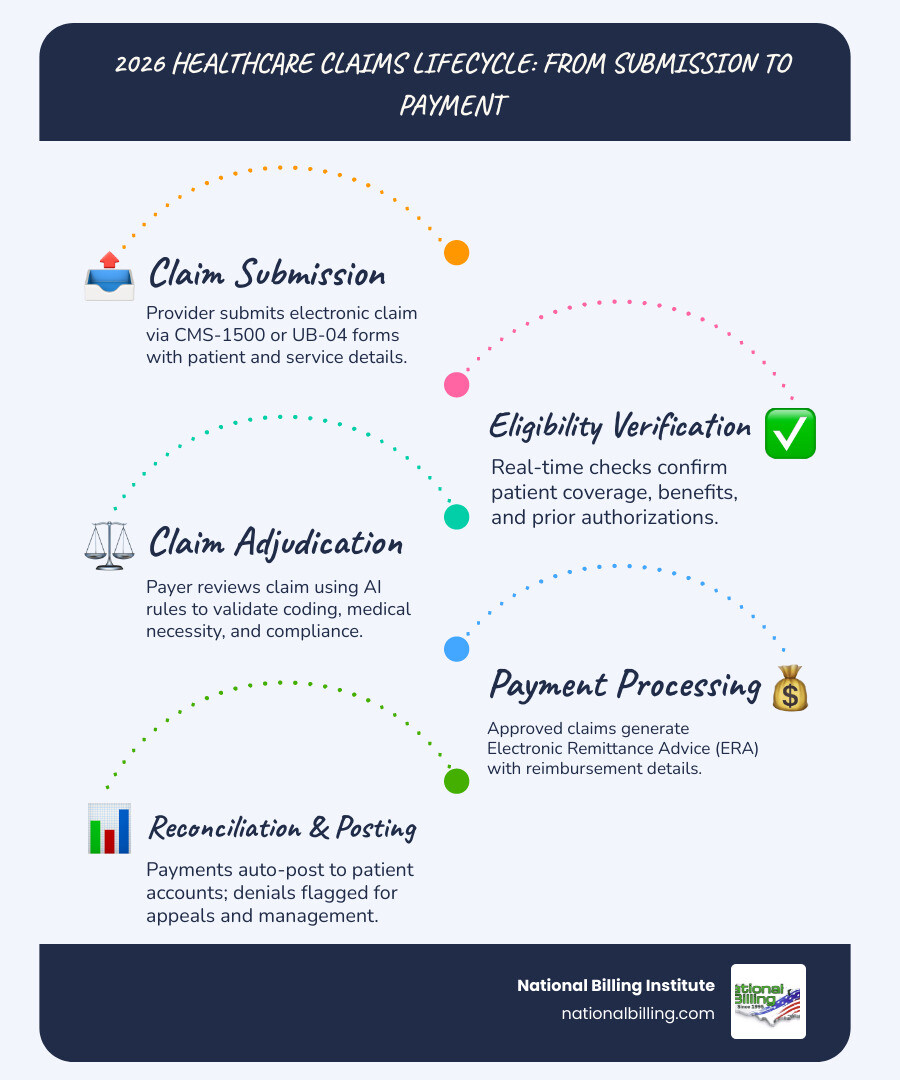
At its simplest, claims processing software healthcare platforms act as the digital bridge between a medical provider's service and the insurance payer's checkbook. When we talk about these systems, we are looking at the technology that manages the entire lifecycle of a medical claim - from the moment a patient checks in to the final reconciliation of payment.
The heart of these systems is the adjudication process. This is the series of steps where a claim is reviewed by the payer to determine if it is valid, how much of the service is covered, and what the final reimbursement should be. Without sophisticated software, this process would be a mountain of paper and manual data entry that would leave most practices in financial ruin.
Modern systems provide robust provider portals that allow us to track every claim in real-time. This visibility is essential for maintaining financial stability. In 2026, these tools are no longer just "nice to have"; they are a requirement for staying compliant with strict HIPAA standards and evolving federal regulations. They ensure that sensitive patient data is encrypted and that every transaction follows the standardized formats required for electronic data interchange (EDI).
Essential Features of Claims Processing Software Healthcare
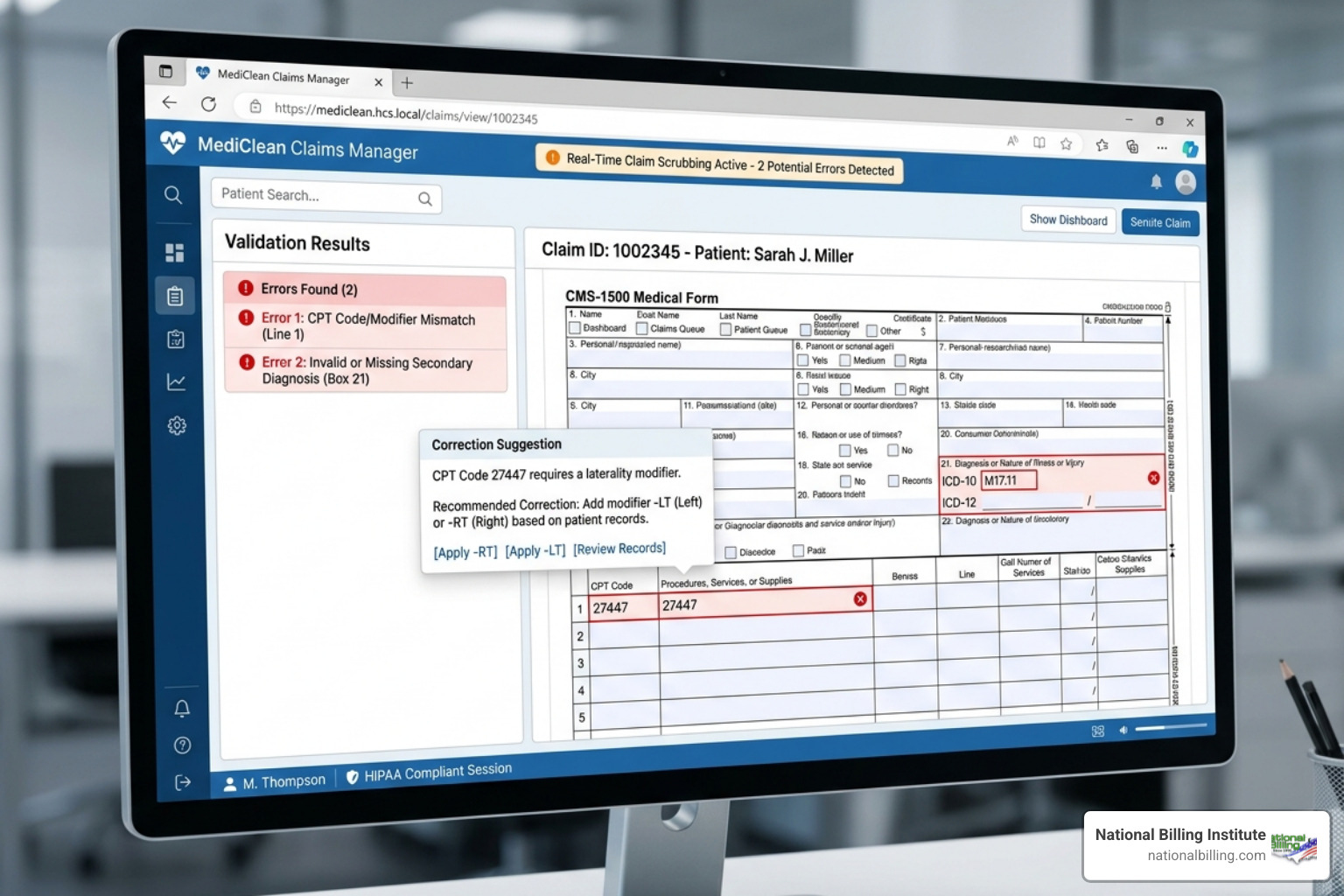
When we evaluate software for our clients, we look for features that actually move the needle on revenue. It isn't just about having a place to type in codes; it's about having a "brain" behind the screen that catches mistakes before they leave your office.
Key Features to Demand:
Real-time Eligibility: You should never provide a service without knowing exactly what the patient's insurance covers. Top-tier software checks eligibility in seconds, often including 1,000 or more checks in standard monthly plans.
Electronic Remittance Advice (ERA): Instead of waiting for paper EOBs in the mail, ERA downloads allow for automatic payment posting. This reduces manual entry errors and speeds up the reconciliation process.
Comprehensive Form Support: The software must handle both CMS-1500 (for professional services) and UB-04 (for institutional claims) seamlessly.
Advanced Denial Management: This is where the best systems shine. By flagging "Certain to Deny" claims through pre-submission edits, some platforms can increase first-pass billing accuracy by 24% to 31%.
At National Billing, we've found that the most effective systems are those that allow for "white-glove" service levels. This is a core part of Why Choose National - we prioritize tools that offer transparent reporting and proactive issue resolution.
Automation in Claims Processing Software Healthcare
By April 2026, the industry has shifted from "AI-added" to "AI-native" workflows. What does this mean for you? It means the software doesn't just wait for you to make a mistake; it uses predictive analytics and rule engines to prevent it.
For example, leading tools use generative AI to create custom claim edits in just three minutes - a task that used to take three days. These clean claim rates (often exceeding 98.5%) are achieved because the software "learns" payer-specific rules and applies them automatically. This level of automation intelligence is the standard for 2026, helping organizations deflect up to 55% of provider inquiry calls by providing clear, automated status updates.
Evaluating Claims Processing Software Healthcare for Your Practice
Choosing the right system requires looking beyond the sales pitch. You need to consider scalability - will this software grow with you if you add three more locations next year?
You should also look closely at:
User Experience: If the interface is clunky, your staff will find workarounds that lead to data silos.
Implementation Timelines: Transitioning to a new system shouldn't take a year. Expert-guided transitions can often happen with minimal disruption to your daily Services.
Pricing Models: In 2026, you'll see everything from "Unlimited" plans at roughly $120/month to "Basic" pay-per-use models at $30/month. Larger organizations often prefer a percentage-of-collections model, which aligns the software provider's success with the practice's revenue.
Payer vs. Provider-Focused Systems
It is a common misconception that all claims software is the same. In reality, there is a massive divide between systems built for the people sending the bills (Providers) and those built for the people paying them (Payers).
Feature Provider-Focused (Billing) Payer-Focused (Admin) Primary Goal Maximize Reimbursement Accurate Adjudication Core Function Claim Scrubbing & Submission Benefit Design & Enrollment Key Metric Days in A/R Operational Efficiency / Auto-adjudication Data Focus Clinical Documentation / ICD-10 Member Eligibility / Plan Limits
Payer systems focus on core administration. They manage complex member enrollments, dental and vision plan designs, and high-speed auto-adjudication. Provider systems are designed to catch coding errors and track the status of a claim until the money hits the bank.
Payers are increasingly consolidating these platforms to manage multiple business lines (like Medicaid and Medicare) in one unified environment, often seeking 99.999% uptime to ensure constant connectivity with their provider networks.
Benefits of Modern Claims Management
The shift toward integrated, AI-driven claims processing software healthcare has created a "new normal" for financial performance. We are no longer just hoping a claim gets paid; we are engineering it to be paid.
The benefits of upgrading to a modern system include:
Faster Payments: By reducing the time a claim sits in "pending" or "rejected" status, practices can see revenue increases of 15% to 30%.
Reduced Administrative Friction: Automation cuts down on manual data entry and "re-keying," which are the primary sources of human error in medical billing.
Cash Flow Optimization: Systems that offer proactive monitoring can identify payer issues before they impact your finances, moving claims from submission to payment in record time.
Error Reduction: With 2.5 million continuously updated edits in some top-tier systems, the likelihood of a clinical denial is virtually eliminated.
One healthcare payer reported a 7.61x increase in operational efficiency simply by replacing an outdated, siloed system with a modern, integrated platform. That is the kind of impact the right technology can have.
Frequently Asked Questions about Claims Systems
What are the common pricing models for claims software in 2026?
Pricing has become much more flexible.
Subscription Fees: Flat monthly rates (e.g., $60 to $120/month) are popular for small to mid-sized practices.
Per-Claim Pricing: A "pay-as-you-go" model for very low-volume providers.
Percentage of Collections: Common for full-service RCM solutions where the software and billing service take a small cut (usually 3-9%) of what they successfully collect for you.
Enterprise Licensing: Custom quotes for large health systems or payers that require massive data throughput and thousands of users.
How does claims software integrate with existing EHRs?
In 2026, API-driven connectivity is the gold standard. Modern claims systems use HL7 standards and secure APIs to "talk" to your Electronic Health Record (EHR) and Practice Management (PM) systems. This ensures a seamless data flow—when a clinician finishes a note in the EHR, the billing data is automatically pulled into the claims software without anyone having to type it twice.
What security certifications should I look for?
Security is non-negotiable. At a minimum, look for HIPAA compliance and SOC II certification. High-performance platforms often carry HITRUST e1 certification, which demonstrates a foundational level of cybersecurity. Always ensure that data is encrypted both "in transit" (as it travels to the payer) and "at rest" (while it sits on the server).
Conclusion
Choosing the right claims processing software healthcare platform is a high-stakes decision, but you don't have to make it alone. The landscape in 2026 is filled with powerful, AI-driven tools that can transform a struggling revenue cycle into a high-performance engine.
At National Billing Institute, we combine these cutting-edge technologies with our 100% USA-based team in Boca Raton, FL. With over 30 years of experience, we specialize in AI-automated processing that delivers the lowest denial rates in the industry and helps our clients see a 15-30% revenue increase.
Ready to see how your current system stacks up? Schedule Billing Review with our experts today and let us help you find the path to peak financial performance.