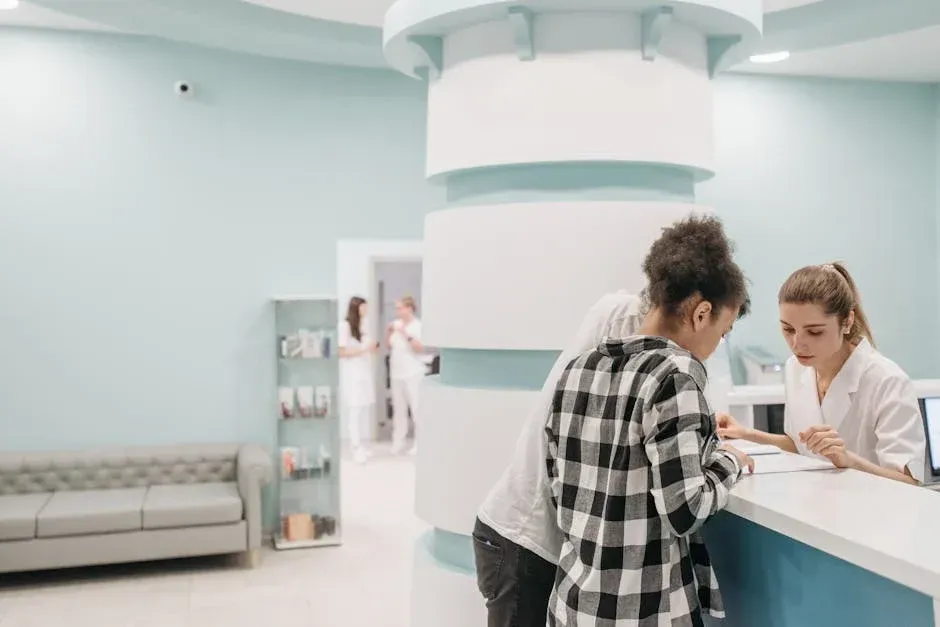
How A/R Follow Up Services Save Your Bottom Line
Why Uncollected Claims Are Quietly Draining Your Practice's Revenue
A/R follow up services are specialized billing solutions that track, recover, and resolve unpaid or denied insurance claims — so healthcare providers get paid for work they've already done.
Here's what A/R follow-up services typically do:
Track outstanding claims across all payers and aging buckets
Identify and resolve denied, underpaid, or delayed claims
Resubmit corrected claims and file appeals on your behalf
Follow up directly with insurers and patients until payment is received
Provide reporting on collection rates, denial trends, and days in A/R
If you run a medical practice, you already know the frustration: you provide care, you submit a claim, and then... nothing. Or worse, a denial.
Claims that don't get followed up on don't just sit there — they disappear. Industry data from organizations like the Healthcare Financial Management Association (HFMA) shows that claims lingering past 60 to 90 days become increasingly difficult to collect. And once you pass the 90-day mark, many payers begin approaching their timely filing limits.
The financial damage adds up fast. Healthcare providers lose thousands in revenue every year simply because aging claims go unfollowed. When A/R days creep above 40, the financial pressure on your practice grows — and your team's bandwidth to chase claims shrinks at exactly the wrong time.
It's a cycle that's hard to break without the right system in place.
I'm Olivia Harper, Founder and Denial Management & Reimbursement Specialist at National Billing Institute, with over 30 years of hands-on experience delivering A/R follow up services for practices across the United States. In that time, I've seen how the right follow-up process can be the difference between a thriving practice and one that's quietly hemorrhaging revenue.
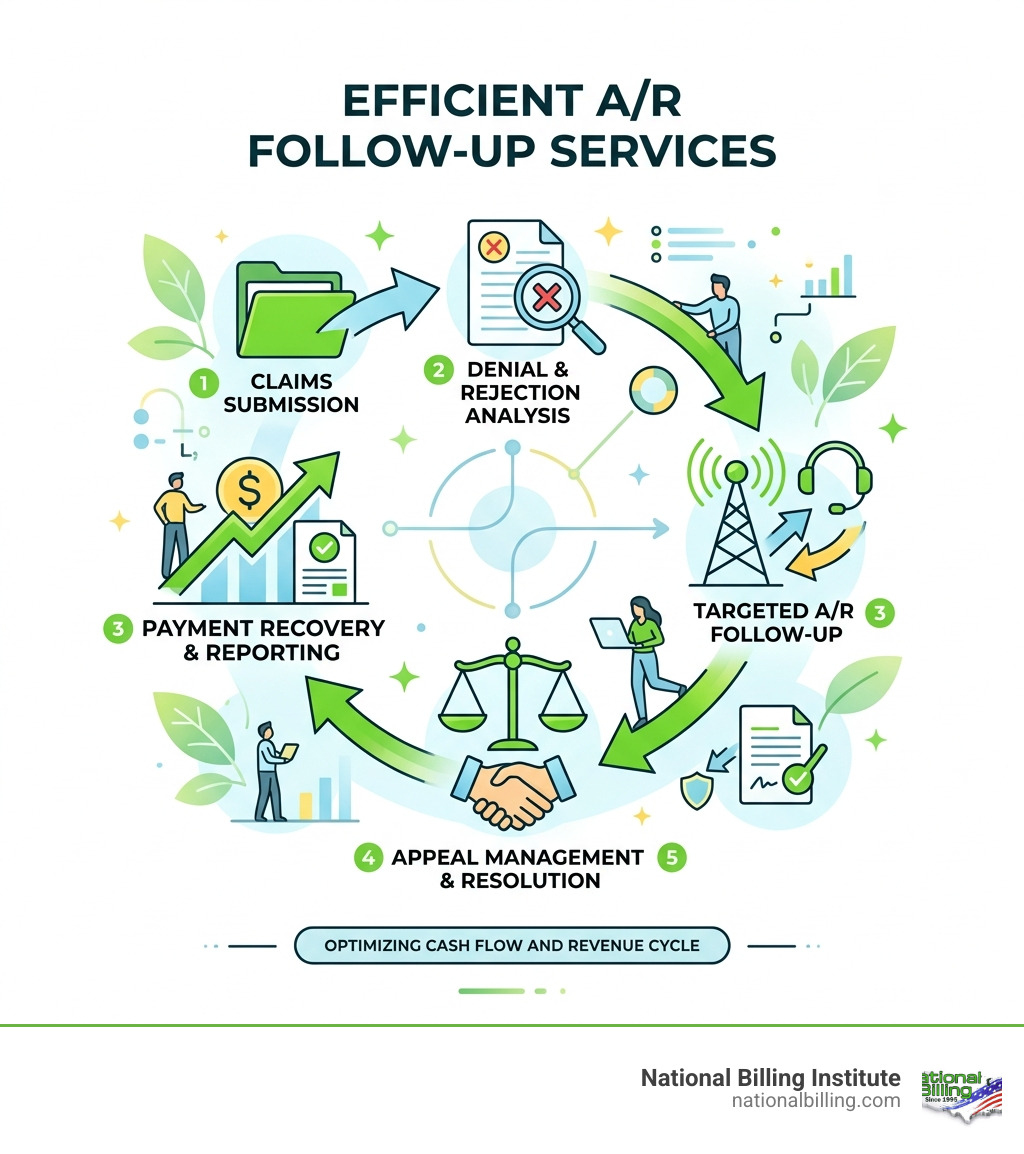
The Critical Role of A/R Follow-Up Services in Medical Billing

In the complex world of healthcare finance, Accounts Receivable (A/R) represents the lifeblood of your practice. It is the money owed to you by insurance companies and patients for services you have already rendered. However, "owed" is not the same as "in the bank."
Effective a/r follow up services ensure that the gap between providing care and receiving payment is as narrow as possible. Ideally, claims should be resolved within 30 to 45 days. Once a claim crosses the 60 or 90-day threshold, the statistical likelihood of it being paid drops significantly. We often see that if A/R days exceed 40, the financial pressure on a practice increases exponentially, limiting your team's capacity to focus on patient care.
At National Billing, we view A/R management not just as a "to-do" list, but as a comprehensive methodology. This includes analyzing insurance contracts, monitoring collection ratios, and preventing "revenue leakage"—those small, overlooked denials that add up to thousands of dollars in lost income every year. To see how we can plug these leaks, explore our full range of medical billing services.
Why Effective A/R Management is Critical for Providers
In an era of declining reimbursement rates and rising operating costs, you cannot afford to leave money on the table. Effective A/R management is the difference between financial stability and constant cash flow stress.
When we take over A/R for a practice, we focus on:
Maximizing Realized Revenue: Ensuring every dollar earned is actually collected.
Reducing Denial Rates: Identifying why claims are being rejected and fixing the root cause.
Preventing Bad Debt: Moving claims through the system before they become uncollectible.
Contract Analysis: Ensuring payers are actually paying the rates they agreed to in your contracts.
Common Challenges in Managing Accounts Receivable
Why is this so hard to do in-house? Because the "goalposts" for insurance claims are constantly moving. Common hurdles include:
Coding Errors: A single digit wrong on a CPT or ICD-10 code can delay payment by 45 days.
Documentation Gaps: Payers often "pend" claims, asking for more medical records, which then sit in a stack on someone's desk.
Staffing Shortages: Chasing a $50 claim for three hours isn't a great use of a high-paid office manager's time, so it often doesn't happen.
Payer Complexity: Every insurer has different "timely filing" limits, ranging from 90 days to a year. If you miss the window, the money is gone forever.
A Step-by-Step Guide to Recovering Outstanding Medical Claims
Recovering money shouldn't be a guessing game. It requires a systematic, proactive approach. Here is the workflow we use at National Billing to ensure no claim is left behind.
Assessment & Prioritization: We don't just start at the top of the list. We prioritize claims by value, payer history, and—most importantly—impending timely filing deadlines.
Claim Scrubbing & Verification: Before a claim even goes out (or when we are reworking a denied one), we verify eligibility in real-time.
Daily Follow-Up: Whether via payer portals, phone calls, or automated inquiries, we touch outstanding accounts daily.
Payment Posting & Secondary Filing: Once the primary payer pays, the clock starts on the secondary insurance. We ensure this transition happens instantly.
Manual vs. Automated Follow-Up Workflows
Feature Manual Follow-Up (In-House) Automated & Expert Follow-Up (National Billing) Speed 14+ hours/week spent chasing Real-time, 24/7 monitoring Error Rate High (Human fatigue/oversight) Low (AI-driven scrubbing) DSO (Days Sales Outstanding) Often 50-60+ days Targeted reduction to <35 days Recovery Rate 20-30% of denials 50-70% of denials recovered
If you're curious about where your current process stands, you can schedule a billing review with our team in Boca Raton.
How A/R Follow-Up Services Handle Denials and Appeals
Did you know that 50–70% of denied claims can be successfully recovered with expert intervention? Most in-house teams simply don't have the time to go through the multi-level appeal process.
We perform a root-cause analysis on every denial. Is it a medical necessity issue? A "coordination of benefits" problem? Once we identify the pattern, we don't just fix one claim; we fix the workflow to prevent that denial from ever happening again. We handle the heavy lifting of payer communication, often making 5 to 10 contact attempts for problematic payers to ensure resolution.
The Role of Patient Engagement in Successful Collections
Insurance is only half the battle. As deductibles rise, more of your A/R is likely sitting in "patient due" buckets. We use technology to make this easier for both you and the patient.
Collectability Scoring: We help you understand which accounts are most likely to pay so you can prioritize outreach.
Patient Portals: Giving patients a simple way to see their bill and pay online reduces friction.
Clear Communication: We explain the "why" behind the bill, which leads to faster payments and higher patient satisfaction.
Skip Tracing: If a patient moves without a forwarding address, we use advanced tools to find updated contact info.
Find out more about why to choose National Billing for your patient-facing and insurance-facing collections.
Measuring Success: Metrics and Technology in A/R Management
You can’t manage what you don’t measure. In a/r follow up services, there are three "North Star" metrics we track for every client:
Days in A/R (DSO): The average number of days it takes to get paid. If this is over 40, your practice is in the "danger zone."
Net Collection Rate: What percentage of the "allowed amount" are you actually collecting? We aim for 96% or higher.
Aging Buckets: What percentage of your money is over 60, 90, and 120 days old? Money in the 120+ bucket is often at risk of becoming bad debt.
Leveraging AI and Automation in A/R Follow-Up Services
At National Billing, we combine our 30+ years of experience with cutting-edge AI. Automation isn't about replacing humans; it's about making them "super-human."
35% Faster Resolution: AI-powered workflows can identify "clean" claims and push them through while flagging problematic ones for our experts.
Automated Reminders: Patients get polite, psychologically-tuned reminders that get paid up to 45% faster than a standard paper statement.
EHR/PM Sync: Our systems integrate directly with your existing software (like Epic, Cerner, or Kareo), ensuring real-time data exchange without manual entry.
Future Trends Shaping Healthcare Revenue Cycles
The future of RCM is "predictive." We are moving toward a world where we can predict a denial before the claim is even submitted.
Virtual ARMS: Cloud-based Accounts Receivable Management Systems allow for total transparency. You can see exactly what we are doing, in real-time, from any device.
Automated Voice Outreach: Using AI-driven voice technology to handle routine follow-ups, freeing up human specialists for complex appeals.
Real-Time Eligibility: Verifying coverage before the patient even walks through your door to prevent front-end denials.
Learn more about our company history and mission to stay ahead of these trends.
Strategic Benefits of Outsourcing Your Revenue Cycle
Many providers ask: "Why shouldn't I just hire another person to do this in-house?" The truth is that the cost of an in-house employee—salary, benefits, desk space, and training—is often much higher than the cost of a specialized service.
Outsourcing to a dedicated team can lead to a 30% reduction in administrative costs. But the real value is in the results. Our clients typically see a 15-30% increase in revenue simply because we are focused 100% on your bottom line, not on checking patients in or answering phones.
Furthermore, we provide:
100% USA-Based Teams: Our specialists are right here in Boca Raton, FL. We understand the nuances of the American healthcare system and regional payer trends.
HIPAA Compliance: We maintain the highest levels of data security to protect your practice and your patients.
Scalability: Whether you are a solo practitioner or a multi-site group, our services grow with you.
Ready to see the difference? Contact us for a consultation.
Choosing the Right Partner for Your Practice
Don't settle for a "black box" billing company where you never know what's happening with your claims. The right partner should offer:
Full Transparency: You should have access to your data 24/7.
Regular Reporting: We provide weekly and monthly deep dives into your performance.
Regional Expertise: Especially in Florida, where Medicare complexity and "snowbird" populations create unique billing challenges, local knowledge is key.
Proven ROI: If the service doesn't pay for itself through increased collections, it's not the right fit.
Frequently Asked Questions about A/R Follow-Up Services
How long should a claim stay in A/R before becoming problematic?
Ideally, you want to see resolution within 30 to 45 days. Once a claim hits 60 days, it requires active intervention. If it reaches 90 days, it is in the "critical" zone due to timely filing limits. Claims over 120 days often represent "lost" revenue unless handled by a specialized recovery team.
What is the typical ROI of outsourcing A/R management?
Most practices see a significant return on investment within the first 90 days. Between reducing administrative overhead (saving about 14 hours of staff time per week) and increasing net collections by 15-30%, the service usually pays for itself many times over.
How do A/R services ensure HIPAA compliance and data security?
At National Billing, we use encrypted, cloud-based platforms and strictly adhere to HIPAA regulations. Our 100% USA-based team undergoes regular security training, and our systems feature full audit trails, ensuring every touchpoint on a patient's account is recorded and secure.
Conclusion
Managing a medical practice is hard enough without having to fight for every dollar you've earned. A/R follow up services aren't just an administrative luxury; they are a strategic necessity for any practice that wants to remain financially healthy in today's healthcare environment.
With over 30 years of experience and a 100% USA-based team in Boca Raton, National Billing Institute is dedicated to helping you achieve the lowest denial rates and the highest possible revenue. We combine the warmth of a local partner with the power of AI-driven automation to ensure your bottom line is protected.
Stop letting your hard-earned revenue vanish into the "aging" bucket. Get started with professional A/R follow up services today and take control of your revenue cycle.