
How to Overturn Denied Claims with Better Appeal Management
Why Denials and Appeals Management Is Costing You More Than You Think
Denials and appeals management is the process healthcare providers use to identify, challenge, and resolve insurance claim denials — so they can recover revenue that would otherwise be lost.
Here's a quick breakdown of what it involves:
Step What It Means Identify Catch denied claims and log them in a central system Categorize Sort by denial type (hard vs. soft) and root cause Prioritize Focus on high-dollar and time-sensitive claims first Appeal Submit documentation to challenge the denial Follow up Track payer responses and escalate when needed Prevent Fix upstream issues so the same denials don't repeat
Claim denials are getting worse. As of April 2026, 73% of revenue cycle leaders report that denials are increasing — up from just 42% in 2022. Payers are automating rejections, changing policies more frequently, and tightening prior authorization rules. The result? More denied claims, slower reimbursements, and growing pressure on already stretched billing teams.
What makes this so damaging is how little gets done about it. 65% of denied claims are never reworked at all — meaning that revenue simply disappears. For many practices, that adds up to 5–25% of total claims sitting in denial limbo.
The good news: most denials are preventable or recoverable with the right process in place.
I'm Olivia Harper, Founder and Denial Management & Reimbursement Specialist at National Billing Institute, and I've spent over 30 years helping healthcare practices across the US build stronger denials and appeals management systems that protect their revenue. In this guide, I'll walk you through exactly what works — from identifying denial types to navigating the Medicare appeals hierarchy to using AI tools that cut appeal time by up to 90%.

Understanding Denials and Appeals Management in 2026
In the current landscape of April 2026, denials and appeals management has shifted from a back-office administrative task to a core pillar of financial survival. With the top five payer companies now controlling over 50% of the health insurance market, their ability to implement automated denial systems has outpaced many providers' manual workflows.
Effective revenue recovery requires more than just "fixing mistakes." It requires a comprehensive Denial Management & Appeals: Guide for Healthcare Providers that treats every denial as a data point. When we see reimbursement times increasing for 67% of providers, we know that the "wait and see" approach is no longer viable. We must treat denials as signals of systemic issues within the revenue cycle, from front-end registration to back-end Clinical Appeals & Denials Management.
The Difference Between Hard and Soft Denials
To manage your workflow effectively, we first have to speak the language of the payers. Not all denials are created equal. We categorize them into two main buckets: Hard and Soft.
Feature Hard Denials Soft Denials Definition Permanent loss of revenue; often considered "final." Temporary denials that can be corrected and paid. Common Causes Lack of Medical Necessity, non-covered services. Missing information, coding errors, eligibility issues. Action Needed Formal clinical appeal with physician involvement. Corrected claim submission or additional documentation. Prevalence Typically 5–10% of total denials. The vast majority of daily billing "hiccups."
Hard denials are the "heavy lifters" of the denial world. They often require a Clinical Appeals & Denials Management strategy because the payer is fundamentally questioning the care provided. Soft denials, often called "administrative denials," are usually the result of a process breakdown that we can fix with better data entry or faster response times.
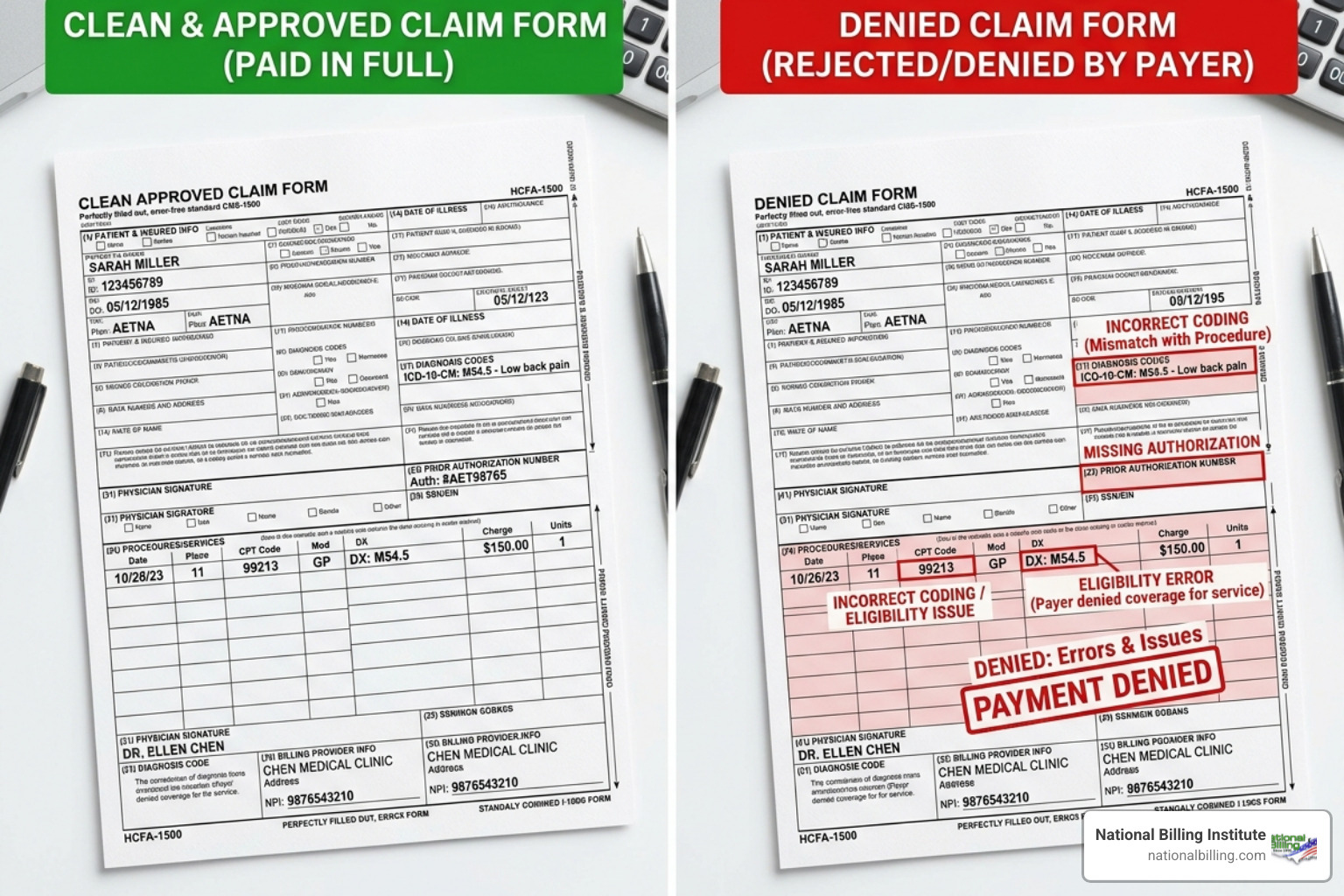
Common Causes of Claim Denials
Why do claims get rejected in the first place? In our experience at National Billing Institute, the "why" usually falls into a few predictable categories:
Registration and Eligibility (22%): This is the most preventable category. If a patient’s insurance has termed or the member ID is entered incorrectly at the front desk, the claim is doomed before the doctor even sees the patient.
Prior Authorization Failures (27%): According to the AMA, nearly 27% of prior authorizations are often or always denied. Payers are increasingly using these as "hoops" to jump through, and missing a single authorization number can lead to an automatic hard denial.
Coding Inaccuracies: Coding mistakes account for a staggering 63% of medical billing errors. Whether it’s failing NCCI edits, using incorrect modifiers, or unbundling codes, these errors are red flags for payer audits.
Timely Filing Limits: Every payer has a "clock." If you don't submit the claim or the appeal within their specific window (often 90 to 120 days), the money is legally gone.
The 7-Step Process for Effective Denials and Appeals Management
To move from reactive "firefighting" to proactive revenue protection, we recommend a structured 7-step lifecycle. This process ensures that no claim falls through the cracks and that your team isn't wasting time on low-value tasks. You can learn more about how we integrate these steps into our Services.
Step 1-3: Identification, Categorization, and Prioritization in Denials and Appeals Management
The first half of the process is all about organization. You cannot fix what you cannot see.
Step 1: Identification: We use centralized tracking to capture every single Electronic Remittance Advice (ERA) or Standard Paper Remit (SPR) that contains a denial code.
Step 2: Categorization: We sort these by the "reason code." Is it a PR (Patient Responsibility) or a CO (Contractual Obligation)? Is it a "soft" demographic error or a "hard" medical necessity issue? According to Denials and Appeals Management | Xsolis, consistent categorization is the only way to perform meaningful trend analysis later.
Step 3: Prioritization: This is where many practices fail. They work denials in the order they arrive. Instead, we prioritize based on fiscal impact. We focus on high-dollar claims and major payers first. If you have a $5,000 surgery denial with a 48-hour appeal window, that takes precedence over a $50 office visit with a 90-day window.
Step 4-7: Preparation, Submission, and Prevention Strategies
Once we know what to work on, we move into action.
Step 4: Preparation: This involves gathering the "ammunition." We collect clinical notes, proof of authorization, and any relevant Appealing Denials | CMS guidelines that support our case.
Step 5: Submission: We submit the appeal using the payer’s preferred method—whether that’s an online portal, fax, or clearinghouse.
Step 6: Follow-up: We don't just "send and pray." We use a "tickler" system to check status every 15–30 days. If a payer hasn't responded within their promised window, we escalate.
Step 7: Prevention: This is the most important step. We take the "lessons learned" from the denial and feed them back to the front-end staff. If we see a spike in eligibility denials from a specific carrier, we retrain the registration team on that carrier's specific portal requirements.
Navigating the Medicare Parts A & B Appeals Hierarchy
Medicare appeals are a different beast entirely. They follow a strict five-level hierarchy, and missing a deadline at any level can end your chance of recovery. If you are dealing with Original Medicare (Fee-for-Service), you must follow the process outlined in the Medicare Parts B Appeals Process.
Level 1: Redetermination: Conducted by the Medicare Administrative Contractor (MAC). You have 120 days to file this after the initial denial.
Level 2: Reconsideration: Conducted by a Qualified Independent Contractor (QIC). This is a "de novo" review, meaning they look at the claim with fresh eyes.
Level 3: Administrative Law Judge (ALJ) Hearing: This is where things get serious. There is usually a minimum "Amount in Controversy" (AIC) required to reach this level (adjusted annually).
Level 4: Appeals Council Review: If you disagree with the ALJ, you can move to the Medicare Appeals Council.
Level 5: Judicial Review: The final stop is U.S. District Court.
For a deep dive into the forms and specific language required for these levels, the official Medicare Appeals Guide is an essential resource for your compliance library.
Timelines and Requirements for Medicare Appeals
Timelines are non-negotiable with Medicare. For a Level 1 Redetermination, you have 120 days from the date you receive the remit. Medicare presumes you received the notice 5 days after the date on the letter.
If you move to Level 2 (Reconsideration), the window shrinks to 180 days. The QIC generally has 60 days to make a decision. One pro-tip: always use the CMS-1696 form if you are appointing a representative to handle the appeal for you; it's valid for one year and covers all levels of the appeal.
Leveraging AI and Automation for Superior Results
In April 2026, manual denials and appeals management is like trying to win a Formula 1 race on a bicycle. Technology is the great equalizer. At National Billing Institute, we’ve seen how AI can transform a struggling practice. For example, using specialized Coding Denial Management Services in Boca Raton allows providers to leverage Robotic Process Automation (RPA) to handle the repetitive "grunt work" of status checks.
The impact of AI is measurable:
90% reduction in the time it takes to create appeal packages.
40% higher overturn rate when using predictive analytics to identify which denials are most likely to be paid.
Real-time eligibility checks that catch errors before the patient leaves the office.
If you’re curious about how your current setup compares, you can Schedule Billing Review with us to see where automation could plug your revenue leaks.
Modernizing Denials and Appeals Management with Technology
Generative AI is the newest tool in our arsenal. It can now autonomously draft payer-specific appeal letters using clinical documentation and prepopulated forms. This isn't just about speed; it's about accuracy. AI doesn't get "denial fatigue" and it doesn't forget to attach a required modifier.
By integrating with payer APIs, we can get "enhanced responses" that provide service-line details and financial breakdowns that standard X12 276/277 transactions often miss. This normalized data allows us to see trends across 450+ payers instantly, rather than logging into dozens of different portals.
Frequently Asked Questions about Claim Denials
What key performance indicators (KPIs) should be tracked?
To know if your denials and appeals management is actually working, you need to track these five industry benchmarks:
Denial Rate: Target < 5%.
Clean Claim Rate: Target > 98%.
Appeal Success Rate: Target > 60%.
Average Days to Resolve: Target < 30 days.
Cost per Denial: This includes staff time and software—aim to keep this as low as possible through automation.
How does patient engagement reduce denials?
It might surprise you, but the patient is a key ally in preventing denials. Demographic errors and "missing information" denials often stem from poor communication. We’ve seen that implementing text message reminders can lead to a 26.6% increase in payments within the first 30 days. When patients have access to a portal and receive clear, transparent billing info, they are more likely to provide the correct insurance data upfront, reducing the chance of a "Member Not Found" denial later.
What role does root cause analysis play?
Root cause analysis is the "detective work" of billing. Instead of just fixing a single denied claim, we ask, "Why did this happen to 50 claims this month?"
Is it a specific doctor's documentation?
Is it a specific front-desk staff member?
Is it a new payer policy that hasn't been updated in our system? By identifying these "process signals," we create a feedback loop that allows us to fix the problem at the source, turning a reactive billing department into a proactive revenue powerhouse.
Conclusion
Managing denials in 2026 is a complex, high-stakes game, but it’s one you can win. By shifting from manual rework to a structured, AI-enhanced denials and appeals management strategy, you can stop leaving money on the table and start focusing on what matters most: your patients.
At National Billing Institute, we take the burden of denials off your shoulders. Based right here in Boca Raton, FL, our 100% USA-based team brings over 30 years of experience to the table. We don't just "process" claims; we fight for every dollar. Our clients typically see a 15–30% increase in revenue and enjoy some of the lowest denial rates in the industry.
Ready to see how much revenue you could be recovering? Explore our full suite of Services or Contact Us today to start your journey toward a healthier revenue cycle.